Breast cancer is a tumour in the breast that contains cancerous cells. A breast tumour is a lump created by an abnormal and uncontrolled growth of cells. It can either be malignant (cancerous) or benign (not cancerous).
The breasts
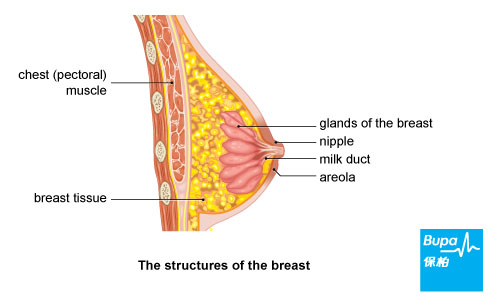
Breasts are made up of fat, connective tissue and gland tissue divided into lobes. The lobes are connected to your nipple by ducts.
Most women have breasts of different sizes which look and feel different at certain times of the month, depending on their menstrual cycle. Your breasts also change during the different stages of your life, for example, after the menopause, they become less full or dense.
Breast tissue goes into your armpit where there are lymph nodes. These are glands that are part of your immune system.
Breast cancer usually starts in the cells lining the ends of the lobes and in the ducts themselves. It can spread from there into the breast tissue and lymph nodes.
Most women have breasts of different sizes which look and feel different at certain times of the month, depending on their menstrual cycle. Your breasts also change during the different stages of your life, for example, after the menopause, they become less full or dense.
Breast tissue goes into your armpit where there are lymph nodes. These are glands that are part of your immune system.
Breast cancer usually starts in the cells lining the ends of the lobes and in the ducts themselves. It can spread from there into the breast tissue and lymph nodes.
Types of breast cancer
There are a number of different types of breast cancer, including some rare types, such as inflammatory breast cancer and Paget's disease. However, there are two main types of breast cancer. These are described below.
Non-invasive breast cancers
Non-invasive breast cancers are cancers that stay within the ducts or lobes of your breast and don't spread to surrounding tissue or to other parts of the body. The most common type of non-invasive breast cancer is ductal carcinoma in situ (DCIS). This is a very early type of breast cancer where the cancer cells are only found inside the milk ducts and haven't spread into the breast tissue. In some cases, DCIS can develop into an invasive form of breast cancer.
Invasive breast cancers
Invasive breast cancers are cancers that have spread from the ducts or lobes of your breast into the surrounding tissue. The most common type of invasive breast cancer is called invasive ductal carcinoma (IDC), where the cancer cells are in the ducts and the breast tissue. Around eight out of 10 women diagnosed with breast cancer have this type. About one in ten women diagnosed with breast cancer have invasive lobular carcinoma (ILC), which starts growing in the lobes, but can spread to other parts of the breast. Both IDC and ILC can spread to other parts of the body.
Non-invasive breast cancers
Non-invasive breast cancers are cancers that stay within the ducts or lobes of your breast and don't spread to surrounding tissue or to other parts of the body. The most common type of non-invasive breast cancer is ductal carcinoma in situ (DCIS). This is a very early type of breast cancer where the cancer cells are only found inside the milk ducts and haven't spread into the breast tissue. In some cases, DCIS can develop into an invasive form of breast cancer.
Invasive breast cancers
Invasive breast cancers are cancers that have spread from the ducts or lobes of your breast into the surrounding tissue. The most common type of invasive breast cancer is called invasive ductal carcinoma (IDC), where the cancer cells are in the ducts and the breast tissue. Around eight out of 10 women diagnosed with breast cancer have this type. About one in ten women diagnosed with breast cancer have invasive lobular carcinoma (ILC), which starts growing in the lobes, but can spread to other parts of the breast. Both IDC and ILC can spread to other parts of the body.
Causes of breast cancer
The cause of breast cancer isn't yet fully understood. However, there are certain factors that make developing breast cancer more likely. You're more likely to develop breast cancer if you:
- are over 50 and have had either benign or malignant breast cancer before
- started your periods early or your menopause late
- have been exposed to radiation
- had a first pregnancy after the age of 30, or don't have children
- eat a lot of high-fat foods or drink more than the recommended limit of 14 units a week of alcohol
- are overweight and have been through the menopause
- have a close family member who has had breast cancer
- take the contraceptive pill or hormone replacement therapy (HRT), though this increased risk is small
Symptoms of breast cancer
Some women don't notice any changes in their breasts and breast cancer is found when they go for breast screening.
However, many women notice a breast lump or a change in the overlying skin or nipple. About nine out of 10 breast lumps aren't cancer, but if you do find a lump, you should see your doctor straightaway. There are also other symptoms to look out for:
However, many women notice a breast lump or a change in the overlying skin or nipple. About nine out of 10 breast lumps aren't cancer, but if you do find a lump, you should see your doctor straightaway. There are also other symptoms to look out for:
- a change in the shape or size of your breasts
- a different shape to your nipple - for example, it may turn inwards or become irregular in shape
- dimpled skin
- a rash on or around your nipple
- blood-stained discharge from your nipple
- swelling or a lump in your armpit
Diagnosis of breast cancer
Your doctor will ask about your symptoms and examine you. He or she may also ask you about your medical history and examine your breasts.
Your doctor may refer you to a specialist breast clinic where you're likely to have further tests. The most common tests are listed below.
Your doctor may refer you to a specialist breast clinic where you're likely to have further tests. The most common tests are listed below.
- Ultrasound scan or mammogram. An ultrasound scan uses sound waves to produce an image of the inside of the body/or part of the body. This is usually done if you're under the age of 35. A mammogram is an X-ray image of your breasts.
- Biopsy. Your doctor will take a small sample of tissue or cells. This will be sent to a laboratory for testing to determine the types of cells and if these are benign (not cancerous) or cancerous.
Treatment of breast cancer
There are a number of different treatments available for breast cancer and you may have more than one of them. The treatment you have will depend on a number of factors, such as whether or not you have been through the menopause, what type of cancer you have and how advanced it is, and whether your cancer has spread. Your doctor will talk to you about the treatments available to you.
Surgery
The first treatment for most people with breast cancer is usually surgery. Depending on the size and position of your breast lump, your surgeon may suggest either a lumpectomy or a mastectomy. A lumpectomy is where the lump is removed, usually with some healthy tissue around it. A mastectomy is where the whole of your affected breast is removed. You may be offered surgery to have your breast reconstructed afterwards.
With both of these procedures, some lymph nodes may also be removed from your armpit. This is to see whether the cancer has spread.
After surgery, you may have other treatments, such as radiotherapy. You will need radiotherapy if you have had a lumpectomy, but it's less common after mastectomy. These treatments can help to reduce the chance of the cancer coming back or spreading.
Radiotherapy
Radiotherapy is a treatment to destroy cancer cells with radiation. A beam of radiation is targeted on the cancerous cells, which shrinks the tumour.
Radiotherapy is often used to treat breast cancer, usually after surgery. You're likely to need a course of radiotherapy that lasts for three to five weeks. Radiotherapy is given as an out-patient treatment and each treatment only takes a few minutes but you will need to attend five days a week.
Chemotherapy
Chemotherapy uses medicines to destroy cancer cells. You may have chemotherapy:
Hormone therapy
Hormones, such as oestrogen, can affect the growth of breast cancer cells. Taking medicines that block these hormones can treat some kinds of breast cancer. Hormone therapies are usually used after you have had surgery, though they can be used before surgery or to treat cancer that has come back.
Women usually take hormonal treatments for at least five years following initial treatment for breast cancer. There are several types of hormone therapy. Your doctor will help you to choose the right medicine for you.
Biological therapies (monoclonal antibodies)
Biological therapy is treatment with a substance that stimulates your body to attack or control the growth of cancer cells. Antibodies are proteins produced by your immune system that usually fight against bacteria and viruses. Monoclonal antibodies are made in a laboratory and are designed to seek out particular cells.
The most commonly used biological therapy is called trastuzumab (Herceptin). It works by targeting breast cancer cells that have a particular protein on their surface.
Trastuzumab is given into your vein via a drip. You will need to have it every three weeks for a year.
Not all women respond to treatment with biological therapies.
After your treatment
After your treatment has finished, your doctor will ask you to have regular check-ups. He or she will ask if you have any symptoms and may also arrange for you to have blood tests and mammograms. This is to check for signs of the cancer coming back.
If you're well, you will need fewer check-ups as time goes on. If you have any symptoms in between your appointments or are worried at all, speak to your doctor.
Surgery
The first treatment for most people with breast cancer is usually surgery. Depending on the size and position of your breast lump, your surgeon may suggest either a lumpectomy or a mastectomy. A lumpectomy is where the lump is removed, usually with some healthy tissue around it. A mastectomy is where the whole of your affected breast is removed. You may be offered surgery to have your breast reconstructed afterwards.
With both of these procedures, some lymph nodes may also be removed from your armpit. This is to see whether the cancer has spread.
After surgery, you may have other treatments, such as radiotherapy. You will need radiotherapy if you have had a lumpectomy, but it's less common after mastectomy. These treatments can help to reduce the chance of the cancer coming back or spreading.
Radiotherapy
Radiotherapy is a treatment to destroy cancer cells with radiation. A beam of radiation is targeted on the cancerous cells, which shrinks the tumour.
Radiotherapy is often used to treat breast cancer, usually after surgery. You're likely to need a course of radiotherapy that lasts for three to five weeks. Radiotherapy is given as an out-patient treatment and each treatment only takes a few minutes but you will need to attend five days a week.
Chemotherapy
Chemotherapy uses medicines to destroy cancer cells. You may have chemotherapy:
- before your surgery - to shrink the tumour
- after surgery - to reduce the chance of cancer coming back or spreading
- as a treatment for breast cancer that has spread or come back
Hormone therapy
Hormones, such as oestrogen, can affect the growth of breast cancer cells. Taking medicines that block these hormones can treat some kinds of breast cancer. Hormone therapies are usually used after you have had surgery, though they can be used before surgery or to treat cancer that has come back.
Women usually take hormonal treatments for at least five years following initial treatment for breast cancer. There are several types of hormone therapy. Your doctor will help you to choose the right medicine for you.
Biological therapies (monoclonal antibodies)
Biological therapy is treatment with a substance that stimulates your body to attack or control the growth of cancer cells. Antibodies are proteins produced by your immune system that usually fight against bacteria and viruses. Monoclonal antibodies are made in a laboratory and are designed to seek out particular cells.
The most commonly used biological therapy is called trastuzumab (Herceptin). It works by targeting breast cancer cells that have a particular protein on their surface.
Trastuzumab is given into your vein via a drip. You will need to have it every three weeks for a year.
Not all women respond to treatment with biological therapies.
After your treatment
After your treatment has finished, your doctor will ask you to have regular check-ups. He or she will ask if you have any symptoms and may also arrange for you to have blood tests and mammograms. This is to check for signs of the cancer coming back.
If you're well, you will need fewer check-ups as time goes on. If you have any symptoms in between your appointments or are worried at all, speak to your doctor.
Treatment of breast cancer
There are a number of different treatments available for breast cancer and you may have more than one of them. The treatment you have will depend on a number of factors, such as whether or not you have been through the menopause, what type of cancer you have and how advanced it is, and whether your cancer has spread. Your doctor will talk to you about the treatments available to you.
Surgery
The first treatment for most people with breast cancer is usually surgery. Depending on the size and position of your breast lump, your surgeon may suggest either a lumpectomy or a mastectomy. A lumpectomy is where the lump is removed, usually with some healthy tissue around it. A mastectomy is where the whole of your affected breast is removed. You may be offered surgery to have your breast reconstructed afterwards.
With both of these procedures, some lymph nodes may also be removed from your armpit. This is to see whether the cancer has spread.
After surgery, you may have other treatments, such as radiotherapy. You will need radiotherapy if you have had a lumpectomy, but it's less common after mastectomy. These treatments can help to reduce the chance of the cancer coming back or spreading.
Radiotherapy
Radiotherapy is a treatment to destroy cancer cells with radiation. A beam of radiation is targeted on the cancerous cells, which shrinks the tumour.
Radiotherapy is often used to treat breast cancer, usually after surgery. You're likely to need a course of radiotherapy that lasts for three to five weeks. Radiotherapy is given as an out-patient treatment and each treatment only takes a few minutes but you will need to attend five days a week.
Chemotherapy
Chemotherapy uses medicines to destroy cancer cells. You may have chemotherapy:
Hormone therapy
Hormones, such as oestrogen, can affect the growth of breast cancer cells. Taking medicines that block these hormones can treat some kinds of breast cancer. Hormone therapies are usually used after you have had surgery, though they can be used before surgery or to treat cancer that has come back.
Women usually take hormonal treatments for at least five years following initial treatment for breast cancer. There are several types of hormone therapy. Your doctor will help you to choose the right medicine for you.
Biological therapies (monoclonal antibodies)
Biological therapy is treatment with a substance that stimulates your body to attack or control the growth of cancer cells. Antibodies are proteins produced by your immune system that usually fight against bacteria and viruses. Monoclonal antibodies are made in a laboratory and are designed to seek out particular cells.
The most commonly used biological therapy is called trastuzumab (Herceptin). It works by targeting breast cancer cells that have a particular protein on their surface.
Trastuzumab is given into your vein via a drip. You will need to have it every three weeks for a year.
Not all women respond to treatment with biological therapies.
After your treatment
After your treatment has finished, your doctor will ask you to have regular check-ups. He or she will ask if you have any symptoms and may also arrange for you to have blood tests and mammograms. This is to check for signs of the cancer coming back.
If you're well, you will need fewer check-ups as time goes on. If you have any symptoms in between your appointments or are worried at all, speak to your doctor.
Surgery
The first treatment for most people with breast cancer is usually surgery. Depending on the size and position of your breast lump, your surgeon may suggest either a lumpectomy or a mastectomy. A lumpectomy is where the lump is removed, usually with some healthy tissue around it. A mastectomy is where the whole of your affected breast is removed. You may be offered surgery to have your breast reconstructed afterwards.
With both of these procedures, some lymph nodes may also be removed from your armpit. This is to see whether the cancer has spread.
After surgery, you may have other treatments, such as radiotherapy. You will need radiotherapy if you have had a lumpectomy, but it's less common after mastectomy. These treatments can help to reduce the chance of the cancer coming back or spreading.
Radiotherapy
Radiotherapy is a treatment to destroy cancer cells with radiation. A beam of radiation is targeted on the cancerous cells, which shrinks the tumour.
Radiotherapy is often used to treat breast cancer, usually after surgery. You're likely to need a course of radiotherapy that lasts for three to five weeks. Radiotherapy is given as an out-patient treatment and each treatment only takes a few minutes but you will need to attend five days a week.
Chemotherapy
Chemotherapy uses medicines to destroy cancer cells. You may have chemotherapy:
- before your surgery - to shrink the tumour
- after surgery - to reduce the chance of cancer coming back or spreading
- as a treatment for breast cancer that has spread or come back
Hormone therapy
Hormones, such as oestrogen, can affect the growth of breast cancer cells. Taking medicines that block these hormones can treat some kinds of breast cancer. Hormone therapies are usually used after you have had surgery, though they can be used before surgery or to treat cancer that has come back.
Women usually take hormonal treatments for at least five years following initial treatment for breast cancer. There are several types of hormone therapy. Your doctor will help you to choose the right medicine for you.
Biological therapies (monoclonal antibodies)
Biological therapy is treatment with a substance that stimulates your body to attack or control the growth of cancer cells. Antibodies are proteins produced by your immune system that usually fight against bacteria and viruses. Monoclonal antibodies are made in a laboratory and are designed to seek out particular cells.
The most commonly used biological therapy is called trastuzumab (Herceptin). It works by targeting breast cancer cells that have a particular protein on their surface.
Trastuzumab is given into your vein via a drip. You will need to have it every three weeks for a year.
Not all women respond to treatment with biological therapies.
After your treatment
After your treatment has finished, your doctor will ask you to have regular check-ups. He or she will ask if you have any symptoms and may also arrange for you to have blood tests and mammograms. This is to check for signs of the cancer coming back.
If you're well, you will need fewer check-ups as time goes on. If you have any symptoms in between your appointments or are worried at all, speak to your doctor.
Disclaimer
This information was published by Bupa Group's Health Content Team and has been reviewed by appropriate medical or clinical professionals. To the best of their knowledge the information is current and based on reputable sources of medical evidence, however Bupa (Asia) Limited makes no representation or warranty as to the completeness or accuracy of the Content.
The information on this page, and any information on third party websites referred to on this page, is provided as a guide only. It should not be relied upon as a substitute for professional medical advice, nor is it intended to be used for medical diagnosis or treatment. Bupa (Asia) Limited is not liable for any loss or damage you suffer arising out of the use of, or reliance on, the information.
Third party websites are not owned or controlled by Bupa and any individual may be able to access and post messages on them. Bupa is not responsible for the content or availability of these third party websites. Last updated August 2017.
The information on this page, and any information on third party websites referred to on this page, is provided as a guide only. It should not be relied upon as a substitute for professional medical advice, nor is it intended to be used for medical diagnosis or treatment. Bupa (Asia) Limited is not liable for any loss or damage you suffer arising out of the use of, or reliance on, the information.
Third party websites are not owned or controlled by Bupa and any individual may be able to access and post messages on them. Bupa is not responsible for the content or availability of these third party websites. Last updated August 2017.










